16 Jul Heel Pain
Heel Pain Series- Week 2: What is a Podiatrist going to do?
https://www.sportspodiatry.com.au/services/
Plantar fasciitis, heel spur, or something else?
Correct diagnosis is the KEY! How are you meant to treat something if you don’t know what it is? You are essentially guessing. There is plenty that can go wrong in the body to give you heel pain. So how does a podiatrist assess this?
· First- we listen. You are going to give us clues for us to investigate. Tell us how long you have been in pain when it hurts, how bad it hurts, what flares it up, and what helps relieve it. No doubt you have tried some stuff yourself before you come to visit us, tell us all about what has worked and not worked for you. Bring in your shoes and tell us what you get up to every day. Your pain is probably holding you back from things you want to do, so let’s work together and get this thing sorted.
How do you take care of newborn babies’ feet?
· Next we poke, we prod and we assess. We will use all of our anatomy knowledge and your clues to narrow things down. We have ways of checking your blood flow, sensation, your strength, quality of movement, and range of movement. Sometimes the pain in your heel is a symptom, an effect. We are going to be busy working with you to find the cause, so be patient and trust the process.
· Sometimes we need to look a little deeper. In Australia, X-Ray and Ultrasound investigations are bulk billed by Medicare (at no cost to you) when referred by a podiatrist. X-Ray is used to look at bones, joints, and their alignment. Ultrasound helps us look closer at the soft tissues, which include fascia, fat pad, tendons, ligaments, and muscles). Sometimes we have to send off for a more detailed image such as MRI or CT scan. All of these types of images are by no means perfect. We have to treat the PERSON, not the PICTURE.
True Story Case Study:
Suzie (name changed for privacy) came into our clinic concerned about the pain in her left heel. It had been going on for over a year now. It made her hobble to the bathroom in the morning but felt ok once she got going. If she stopped again for a short rest, the pain would return. She tried changing her shoes but that didn’t fix it. Suzie went to her GP who had sent her for X-Rays. The Doctor told her she had a heel spur that was causing her pain, and offered her a cortisone injection. The injection was not very pleasant, and annoying it did not resolve her pain. Now if you haven’t spotted it already, have a closer look at the X-Rays.
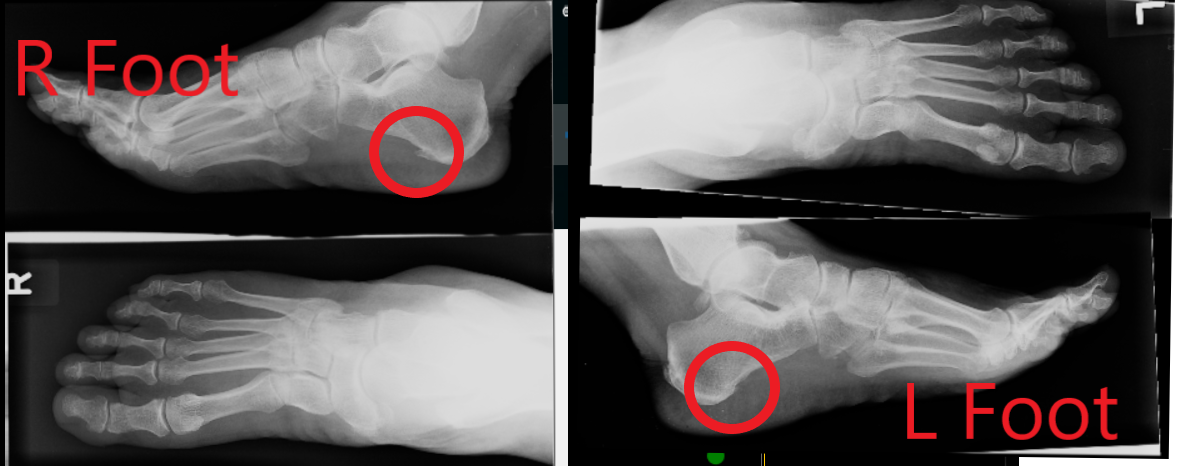
Can you see the spur (the pointy bit) on her right heel bone that I have circled in red? Remember which foot Suzie had her pain in? On her LEFT foot. You can see in the picture, there is little to no change in the heel bone on the left. TAKE HOME MESSAGE: Heel spur does not always equal pain.
So, what did we do? We did exactly what we do for every patient. We listened to her story and how she felt, then we assessed her feet and legs, sitting down and standing up. We did not feel like Suzie’s symptoms were bone-like. She had no night pain and found her pain reduced when she got moving, so it had to be something more elastic than bone. Anyone who has broken a bone will tell you, it does not make it feel better to put pressure on it. Her foot was not hot or red, and her sensation and blood flow was normal. Suzie was so frustrated, she just wanted to get out walking again, to lose a bit of weight for an upcoming holiday.
We wanted to look more closely and test all of Suzie’s soft tissues in the heel area and around the area she is getting pain. We diagnosed Suzie had plantar fasciitis and we started working on her new treatment plan to suit her lifestyle straight away.
Now that we have a diagnosis, let’s talk more about treatment next week…
Talk soon,
Hannah

Sorry, the comment form is closed at this time.